Electroshock therapy in the treatment of depression
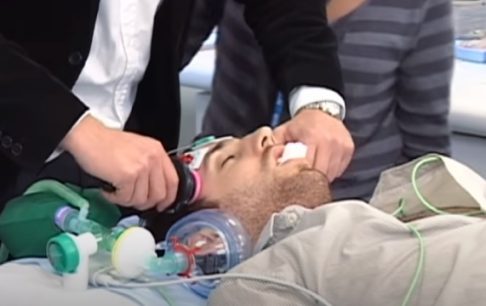

Electroshock therapy – a method of treatment introduced into psychiatry in the first half of the 20th century is still used today. It is used to this day due to its high efficiency. However, the way this therapy is carried out has changed. Today, electroconvulsive therapy is not as dangerous and painful as it used to be.
Electroconvulsive therapy formerly
Electroconvulsive therapy was first used in 1938 by Italian doctors. They applied it to a patient with schizophrenia and achieved relief from symptoms after several treatments.
In those days, electroconvulsive therapy was a painful and dangerous method. The electricity passed through the patient’s head caused a strong epileptic seizure, during which the muscles contracted. As a result, there were occasional tongue bites, jaw dislocations and even bone fractures. The treatments quite often also resulted in cognitive impairments, such as memory problems.
Electroconvulsive therapy nowadays
Currently, electroconvulsive therapy is performed under general anesthesia (the patient is put to sleep for about 10 minutes) and after administration of muscle relaxants, thanks to which such a strong seizure does not occur. The parameters of the passed current have also changed.
Still, electroconvulsive therapy can lead to memory impairment, but they are less common and weaker than in the first half of the 20th century. These include retrograde amnesia, i.e. the amnesia of events preceding the therapy, and anterograde amnesia, i.e. the impairment of the ability to memorize new information. Retrograde amnesia is most related to events in the near-therapy period, and it usually passes within a maximum of 2 months in most patients. Anterograde amnesia disappears faster – in the period of 1-3 weeks after the end of the series of treatments. However, in rare cases, memory impairment may be permanent.
Other side effects of electroconvulsive therapy include headache and muscle aches immediately after the procedure, and a state of foggy or drowsiness, which also passes quickly. Very rare but serious side effects include complications from the cardiovascular system (for example a heart attack or cardiac arrest).
Who can be treated by electroconvulsive therapy
Nowadays, electroconvulsive therapy is mainly used to treat depression, both in unipolar and bipolar disorder (alternating periods of depression and mania), and in the treatment of schizophrenia.
Electroconvulsive therapy is not recommended for all depressed patients, but only for some. This applies to the following groups:
- Patients who have not improved with antidepressants.
- Patients who have drug side effects greater than the potential side effects of electroconvulsive therapy.
- Patients for whom pharmacotherapy is associated with a greater risk than the risk associated with electroconvulsive therapy. This is the case, for example, in pregnant women, in whom antidepressants may be harmful to the baby, and in those with somatic diseases who take medication for the disease which may be dangerous when interacting with antidepressants.
- Patients with very severe depression who are at high risk of life due to increased suicidal tendency or inability to eat, and therefore require treatment that brings results quickly.
The proportion of patients receiving electroconvulsive therapy varies from country to country. This method is most commonly used in the US, Scandinavian countries, New Zealand, Scotland, Australia and Ireland. Poland, like, among others, Russia, Spain, Hungary and the Netherlands are among the countries where this method is rarely used, with only some patients meeting the above criteria.
Polish regulations qualify electroshock therapy to the methods of increased risk. Even though the method of the procedure differs significantly from what it looked like several decades ago, this method is still considered inhumane, not only by patients but also by some doctors. Before being qualified for electroconvulsive therapy, a Polish patient undergoes consultations and tests, not all of which are necessary, but only increase costs. Conducting the therapy is also expensive, due to the cost of the device and the need to involve an anesthesiologist. Most Polish psychiatric departments do not have modern electroconvulsive therapy devices, and there is also a lack of trained personnel*.
What is the effectiveness of electroconvulsive therapy
Electroconvulsive therapy would not last so many years if it were not for its high efficiency. Depending on the study, the authors indicate an effectiveness of 50-90%. For comparison, the effectiveness of antidepressants is estimated at 55-70%.
The advantage of electroconvulsive therapy is the possibility of getting better quickly, unlike drugs, which sometimes only bring the first results after a few weeks of use. As part of electroconvulsive therapy, several or a dozen or so treatments are used, with a frequency of 2-3 weeks, but the first results may appear after the first treatment. In about 50% of patients treated, the therapeutic effect is permanent. In the other half, symptoms of depression return within 6-12 months, which requires repeated treatments.
How electroshock therapy helps
It is not known. For over 70 years of using electroconvulsive therapy, scientists have failed to discover the mechanism of its therapeutic action. They only have a few hypotheses.
One hypothesis is to increase the synthesis and release of neuropeptides and hypothalamic hormones. Others believe that the therapeutic effect may be to reduce the excitability of neurons. Another hypothesis draws attention to the effect on monoamine neurotransmitters and another on the immune system. It is also possible that electroshock therapy helps because it increases neuroplasticity (the formation of connections between neurons and new nerve cells) or by increasing the number of glial cells.
Is it possible to replace electroshocks
In recent years, research has been conducted on other methods of stimulating the brain that would not produce the side effects or anxiety that electroconvulsive therapy still causes. So far, however, without much success.
The most studied of the modern methods is transcranial magnetic stimulation (TMS), which uses a magnetic field instead of an electric current. In principle, this method does not cause an epileptic seizure, and therefore no general anesthesia or muscle relaxants are needed. On the other hand, there is a risk that the seizure will nevertheless be triggered and the patient will then be conscious. The advantage of TMS is that it has no side effects in the form of memory impairment, but the disadvantage is its low effectiveness. The studies carried out so far indicate an effectiveness of 30-40% and a quick recurrence of symptoms. The method is also very expensive, which limits its use to a small number of centers.
Another method that does not cause cognitive impairment is stimulation of the vagus nerve. This method uses an electric current to stimulate the peripheral nerve with electrodes placed under the skin. The method is therefore cumbersome due to the need for a surgical procedure to insert the electrode, and the effectiveness is also not high – 20-50%.
Other methods are also being researched: magnetic shocks (induction of an epileptic seizure with a magnetic field), deep brain stimulation (stimulation with electrodes placed in the brain), and transcranial DC stimulation (direct current stimulation, unlike other methods that use alternating current). However, these methods are too poorly studied to be able to judge their effectiveness and each of them has some drawbacks.
* I tooked this information from a research conducted in 2005. Perhaps something has changed in the last 15 years. If you have any (reliable) information on this subject, feel free to write in the comment below the article.
References
- Hese, R. (2007). Miejsce elektrowstrząsów we współczesnej terapii psychiatrycznej, Psychiatria w Praktyce Ogólnolekarskiej, 1(7), 30-36 (pdf at psychiatria.med.pl)
- Krzywotulski, M. i in. (2013). Analiza retrospektywna skuteczności terapii elektrowstrząsami w depresji lekoopornej. Farmakoterapia w psychiatrii i neurologii, 1, 51-56 (pdf at ipin.edu.pl)
- Palińska, D. i in. (2008). Leczenie elektrowstrząsowe w Polsce w 2005 roku – wyniki ankiety przeprowadzonej w polskich szpitalach psychiatrycznych. Psychiatria Polska, 42(6), 825-839 (pdf at psychiatriapolska.pl)
- Studenna, M. i in. (2011). Czynniki przewidujące skuteczność terapii elektrowstrząsowej. Current Problems of Psychiatry, 12(4), 533-536 (pdf at nieuciekaj.com)
- Wójcik, M. i in. (2014). Skuteczność elektrowstrząsów w depresji psychotycznej u pacjentki po przeszczepie nerek. Psychiatria i Psychoterapia, 10(2), 18-26 (pdf at psychiatriapolska.pl)
- Zyss, T. (2010). Nowe techniki stymulacji elektrycznej i magnetycznej w terapii depresji – porównanie z elektrowstrząsami i farmakoterapią. Psychiatria Polska, 44(6), 853-869 (pdf at psychiatriapolska.pl)
- Leczenie W: Andrew Solomon, Anatomia depresji. Demon w środku dnia. Zysk i S-ka, Poznań, 2004
Author: Maja Kochanowska





Add comment